Its now almost five years since the madness of what my colleague Matt Treacy accurately calls the Covid Panic began in earnest in this country, yet the effects of the unnecessarily prolonged lockdowns remain mostly unexamined by the government.
This seems a deliberate tactic, in my opinion. How else to explain the absurd delay? Simon Harris, the Great Frowner, promised last June that a Covid inquiry would take place before the general election. That didn’t happen, and the excuses are wearing thin, especially given the latest Eurostat report, which shows – once more – that Ireland’s excess deaths rate remains persistently, stubbornly, high.
This is what Eurostat reported for December 2024, when Ireland’s excess mortality was recorded as 11.5% – fourth worst in the EU, with Finland, Luxembourg and Malta, in stark contrast to negative excess death rates in Croatia, Bulgaria and Latvia.
What’s even more interesting, however, is the graph which follows immediately afterwards which shows an inescapable trend for Ireland, and not in a good way. Excess deaths are consistently above the EU average.
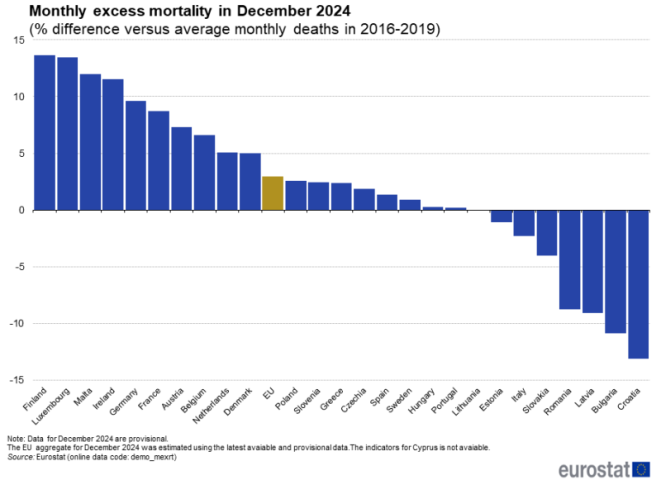
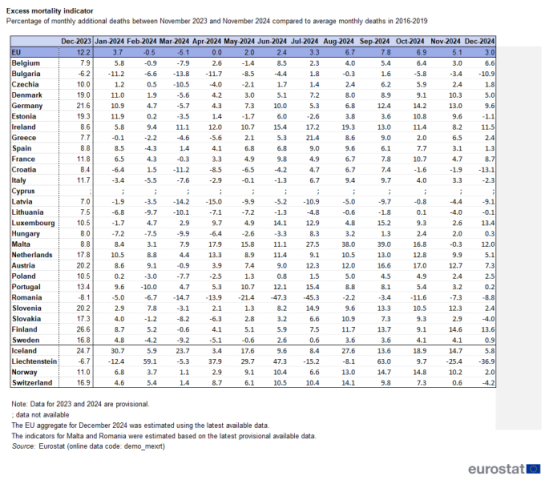
As is evident, Ireland’s excess deaths in the thirteen months to end of December 2024 are sometimes a multiple of the EU average, and are always higher than that average. We are frequently in the top cluster of countries recording significantly high rates of excess mortality.
In fact, the Eurostat data from January 2020 to the end of last year that stark trend – with excess deaths in Ireland very much out of sync with the average for the past two years.
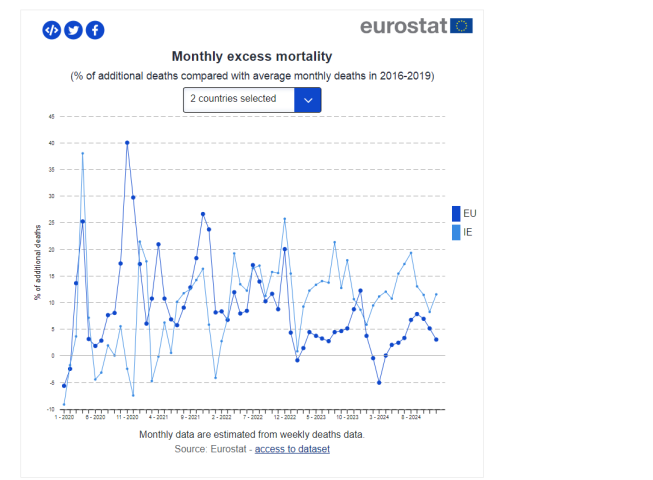
Eurostat notes that excess mortality refers to the number of deaths from all causes measured during a defined period, above that which was observed in the baseline period. The baseline consists of the average number of deaths that occurred in each month during the period 2016-2019, the statistics agency explains.
The higher the value, the higher the number of additional deaths compared with the baseline. A negative indicator shows that fewer deaths occurred in a particular month compared with the baseline period.
This indicator, which is part of the European Statistical Monitor, provides a comprehensive comparison of additional deaths among the European countries. It provides a general measure of mortality because it includes all deaths regardless of their cause
So what is happening? Are more people dying than expected, and if so, why? Did the excessively long Covid lockdowns cause real harm in terms of restricting ability to seek care, especially in regard to screening and early interventions? A report last month from the European Commission found that Ireland has the second-highest rate of new cancer diagnoses in the EU.
Estimated cancer incidence in each country is influenced not only by cancer risk factors but also by the quality of national cancer surveillance systems and cancer screening programmes, the report said.
The profile of cancer in Ireland found 561 new cancer cases per 100,000 women and 733 new cancer cases per 100,000 men were expected in Ireland in 2022.
These figures are both higher than the predicted EU averages of 488 per 100,000 women and 684 per 100,000 men.
Meanwhile, the number of cancer cases is projected to grow by 47% in Ireland from 2022 to 2040, the second highest growth rate in the EU.
It can take time to fully capture the effect of the extraordinary restrictions that were put in place for far too long during Covid. Some earlier studies acknowledged that further data was needed for the full picture to emerge but an October 2024 study published in The Lancet, looking at the effect of the UK lockdown had some grim findings.
There was a substantial decrease in cancer diagnosis during the pandemic, because the period saw a huge-fall off in people seeking help.
Weekly cancer diagnosis rates in 2021 fell by over 60% compared with the mean of the preceding 5 years, the research found – with an estimation that 45% of people with cancer symptoms did not attend their GP in the first lockdown.
“The decline probably resulted from pandemic-related health service disruption, and a reluctance to seek cancer-related medical help, and it is estimated that 45% of individuals with cancer symptoms did not contact their general practitioner during the first lockdown.”
The perceived risk of contracting COVID-19, fear of wasting the doctor’s time, coupled with physical lockdown restrictions and dominant government messaging underscoring the importance of remaining at home were factors in reducing health-care-seeking behaviours. The significant drop in diagnoses suggests many missed cases, potentially of early-stage cancers.
The next finding is really quite profoundly shocking: by the end of the Covid lockdowns, attendance volumes – the number of people attending because of cancer symptoms had fallen by a median of 90%. That is appalling.
Attendance volumes were severely impacted by stringent lockdowns. By the end of the pandemic, attendance volumes had fallen by a median of 90%. Due to the unprecedented decrease in cancer screening and referrals, an increase in missed cancer diagnoses is expected, contributing to this decrease in attendance because of the loss of opportunity to attend.
Simultaneously, pandemic-related service disruptions diminished the capacity for cancer management and treatment. Patients with cancer probably also reduced their health-seeking intent, especially if they considered their condition to be non-urgent.
Conflicting messaging between government and health authorities probably added a further element of confusion for patients already uncertain about seeking care.
That’s a key finding, in my opinion, one that calls to mind the endless doom-announcements during the Covid lockdowns, with newscasters reading out the number of cases daily without the clarification that most people would not be severely impacted by the virus.
The Lancet study spelled out the consequences of this decision to endlessly terrify people:
Decreases in attendance volumes and consultation rates have likely led to delays in cancer diagnoses, treatment, and follow-up. Lower incidence of cancer due to missed or delayed diagnoses have negative effects on cancer-specific mortality, with modelling studies estimating a substantial number of excess years-life-lost.
Patients eventually diagnosed are likely to present with later stage cancer, associated with poorer outcomes. Missed treatments also result in substantial excess mortality in individuals with cancer and other morbidities. We observed an association between attendance decreases and cancer-specific mortality increases.
It seems strange that those same broadcasters and journalists – and most of the politicians in the Dáil – in who hyped up the Covid fear for an entire two years now seem curiously disinterested in excess deaths, whether that’s an attempt to avoid accountability or a refusal to accept that there’s a serious issue that needs to be examined.
One TD told me, off the record, that there’s a significant reluctance to even discuss excess deaths for fear of being seen as seeking to raise issues around vaccine harm. That’s bonkers. All government policies should be open to scrutiny, but the state is being extremely foolish if it thinks that it can dampen down concerns around vaccines, whether valid or not, by ignoring the fact that our excess death rate is a matter of record.
Some factors are certainly important and are now being acknowledged. This week, I asked both the Department of Health and the Society of Actuaries for their insights.
The Department said that excess mortality is a term that refers to estimates of the number of deaths from all causes above and beyond expected under ‘normal’ conditions.
“There are different methods used to estimate the number of deaths ‘normally’ expected. A number of different methodologies have been developed by organisations and academics nationally and internationally to try to estimate levels of excess deaths and it should be noted that estimation methods vary widely. The Department of Health monitors estimates of excess mortality which are published by a range of different sources,” a spokesperson said.
The Health Protection Surveillance Centre (HPSC) has monitored excess mortality in Ireland since 2009, using registered deaths data reported to HPSC on a daily basis from the General Register Office (GRO).
The HPSC participates in EuroMOMO for Ireland, a well-established European mortality monitoring activity. This is the main indicator of excess mortality used in Ireland. The latest estimates from EuroMOMO estimate that Ireland experienced low excess mortality during Winter 2024/2025 for the six weeks from Week 51 2024 to Week 4 2025.
It is important to note that these data are provisional due to the time lag with death registration in Ireland. This means data on excess mortality in recent months will continue to be updated as additional information becomes available.
Eurostat also publishes estimates of excess mortality. They use a different methodology which simply compares the total number of deaths in a specific month with the average deaths in that same month for the baseline years of 2016 to 2019.
The latest Eurostat release estimates that the number of deaths in Ireland during December 2024 was 11.5% higher than the average number of deaths that occurred during December in the years 2016 to 2019.
The Department says that it takes population increase into account and that there has been an increase of 32% in the number of persons aged 65 years and over living in Ireland between 2016 and 2024.
This age group accounts for over 80% of all deaths. The increase in this age group was more than double the 14% increase in the total population over the same period. As of 2024, persons aged 65 years and over account for 15.5% of the population, compared with 13.3% of the population in 2016.
“The extent of the demographic changes in Ireland and the ageing of the population between the baseline period (2016-2019) used by Eurostat, detailed above, and the current year therefore requires caution when comparing the number of deaths in the current period with the average number which occurred during 2016-2019,” it adds.
In addition, The Society of Actuaries in Ireland says that “it appears to us that in [the] Eurostat report, population growth and ageing in recent years haven’t been accounted for.”
“If they haven’t, in the case of a country like Ireland where both of these factors are significant, this would show higher excess deaths than would be the case if those factors were adjusted for,” they said – adding that the data they relied on to assess the impact of the pandemic “relies on us waiting until the deaths have been more fully reported”.
“On that basis we won’t be making any observations on 2024 mortality until late 2026/early 2027,” they said.
It appears then that factors such as an ageing and growing population may be important – but to what extent? And two separate EU bodies giving radically different estimates of excess deaths isn’t going to reassure those who are also reading reports that cancer rates are rising and that the lockdowns caused those with symptoms of disease to miss screenings, appointments, and treatments.
In addition, we seem to have this absurd ongoing situation where Ireland has an unacceptable lag in recording and reporting deaths, causing delays in verifiable information and research.
Clear and decisive answers to these concerns are long overdue. A special task force examining whether or not Ireland is experiencing persistent excess deaths rates, and if we are, what the drivers of that mortality rate might be, should be a priority.