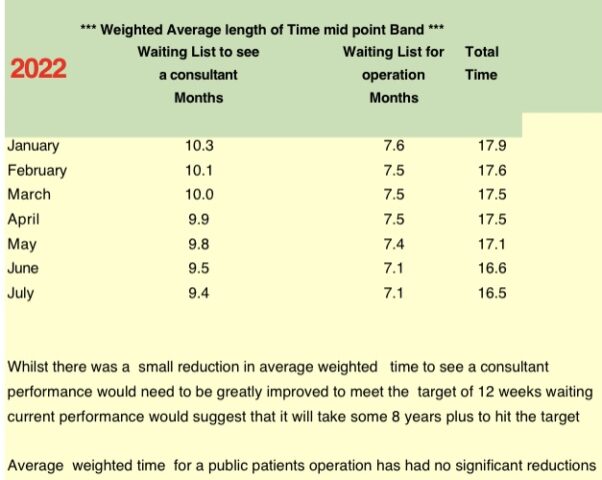
New figures released by the Irish Patients’ Association (IPA) have revealed long waits and overcrowding in emergency departments in Irish hospitals in the past year – something the representative group says is putting patient’s lives at risk.
The patient advocacy group urged for “change and reform” in our healthcare systems that “should not be preceded by preventable funerals and injury to patients” as its research was published this week.
The organisation called for a taskforce to address long public patient wait times, with its figures showing that thousands of people across Ireland are waiting up to two years to see a consultant and have the surgery they need. It said wait times in Ireland are a “public health issue” and safety must be prioritised first, calling on the Minister for Health to take action to implement its recommendations.
The IPA said that for years it has highlighted that patients die or are injured from “preventable errors” while on waiting lists in Ireland, and had repeatedly suggested that monitoring on the impact of waiting lists can be effectively carried out in emergency departments at the time of presentation.
The organisation has also recommended that local doctors monitor their workload associated with public patients attending their practise who are currently on a waiting list.
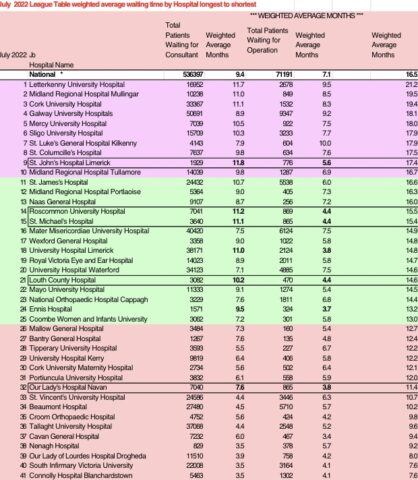
The figures released by the IPA for July revealed that patients in Letterkenny, Cork, Galway, Sligo, and Limerick, are facing the lengthiest wait times to see a consultant and have surgery, with the hospitals in those areas also experiencing emergency department overcrowding in the past year.
The association published its findings in a league table that showed the average wait times to see a consultant and then get surgery in 41 hospitals across Ireland. The waiting times were then combined to provide “average weighted times”.
The data shows that there are massive disparities when individual hospitals are analysed, adding that the national average weighted time is 19.1 months to both see a consultant and have surgery.
The research showed that the longest wait times are at Letterkenny University Hospital, Midlands Regional Hospital in Mullingar, Cork University Hospital, Galway University hospital, and the Mercy University Hospital in Cork. Based on data for July, Letterkenny had the longest wait times for both seeing a consultant for the first time and getting an operation at 21.2-months versus a significantly lower 7.6-months in Blanchardstown.
The data revealed that patients at Letterkenny University Hospital face an 11.7-month wait time to see a consultant and a 9.5 month wait for surgery, equating to a 21.2 month weighted average, which is above the national average. While Midlands Regional Hospital in Mullingar has a 19.5 month weighted average.
The research showed that there are 33,367 patients waiting 11.1 months to see a consultant in Cork University Hospital, which has a weighted average of 19.4. There are also 1,532 people waiting 5.6 months for surgery at the same hospital. The Mercy University Hospital in Cork has an 18-month weighted average to see a consultant and have surgery, while patients at Galway University Hospital also face a lengthy wait time, with an 18.1-month weighted average.
In addition, Galway, Sligo and Letterkenny all experienced “large emergency department overcrowding” in the past year, according to the data:
Wait times are radically different for patients at Cork’s South Infirmary Victoria University Hospital and Connolly Hospital in Blanchardstown – which both have a much lower weighted average waiting time of 7.6-months.
On the publication of the analysis, the IPA urged consultants to remind their public patients who are facing long waits for treatment at home that they can access care faster through the EU Cross-Border directive, under which EU citizens have the right to access healthcare in any EU country and be reimbursed for care abroad by their home country.
The IPA said the new research poses questions which must be answered by the HSE and NTPF.
“We urgently need more real time reporting on the waiting lists performance reporting on the size of the problem (the number) and the length of time (which this analysis highlights) taken together indicate the level of life threatening or quality of life patient safety issues.
“Whilst there is much political focus on the numbers of public patients waiting and subsequent actions and investment to reduce the total numbers there also needs to be hard targets set for reducing the length of time to access public patients care,” it added.
Co-founder of the IPA, Stephen McMahon, also highlighted what he described as “apartheid” in medical care in Ireland – saying that the analysis laid bare inequalities for public patients at many hospitals and again prompts questions about why some hospitals perform better in patient flow than others.
“Acceptance that it will take years as stated in the recent ESRI report on Manpower planning to clear these legacy lists, is merely a continuation of a culture of acceptance that is unacceptable in an economically advanced and skilled society. Such apartheid is not going unseen or unnoticed by the almost 1 million public patients or their families who are experiencing this first hand,” he said.
“The analysis highlights the inequalities for public patients at many Hospitals and once again raises the questions as to why some hospitals do better in patient flow than others. It will be interesting to see other stakeholders,” he said.
The advocacy group also slammed the current patient safety situation as one that is putting patients’ lives at risk, stating that it was time for Health Minister Stephen Donnelly and his department to set up a task force, with an independent chairperson, to be accountable for the management of planned service delivery for public patients.
“We have had enough analysis, descriptions of the problems and false starts all with little overall little progress. Some unfortunate people die, or may have life changing injuries arising from preventable errors in overcrowded emergency departments, the Government / HSE must start to independently monitor all such deaths and injuries to patients in hospitals,” the IPA said.
The IPA has now urged consultants to remind their public patients who are facing long waits that they can access care quicker through the EU Cross-Border directive.
It has also called on the department of health to establish a taskforce, with an independent chairperson, to oversee planned service delivery for public patients.
The new research comes after it was reported earlier this month that 17,000 people died while “languishing on waiting lists” over the last three years in Northern Ireland. The shocking statistics were obtained in an investigation into the scale of the crisis facing Northern Ireland’s hospitals by The Belfast Telegraph. The newspaper accessed the figures through FOI requests sent out to five health trusts in the North.
The figures showed a “huge increase” in the number of people in Northern Ireland dying before they could be treated. The paper reported that waiting lists in the province are the worst in the UK and some of the worst in Europe. It reported that more than 7,600 people died while on a health service waiting list in Northern Ireland last year, with the highest number of deaths being in the Northern Trust area, where 4,269 people died before accessing treatment over a three-year period.
Of this total, 471 people who died waited between three and five years to receive treatment, while an additional 52 people had waited for more than five years. The statistics represent an increase of almost 80% – with the total increasing from 4,310 deaths in 2019 to 7,651 in 2021.
A total of 17,162 people died in Northern Ireland while on a waiting list in the last three years.
The findings sparked anger and were described as “truly staggering” when they were published on 8 August. NI Health Minister Robin Swann has warned that it will take huge funding and up to ten years to fix the crisis in Northern hospitals.
The Belfast Telegraph said that while no suggestion can be made that the deaths were directly related to long waits for treatment, it was clear that many people are spending their last days in “pain and discomfort and without the treatment they need”.